In France, each year, more than 400,000 people burn themselves and for 9,000 of them, these burns are serious. Whatever the cause (a hot liquid or object, electricity, flames, chemicals or even exposure to UV rays), these burns cause significant damage to the skin barrier, making burn victims particularly susceptible to infections.
Indeed, the skin, the largest organ of the human body, is also the first line of defense against bacteria and viruses. Skin tissue is made up of three layers: the epidermis, the dermis and the hypodermis (from the outside to the inside of our body). The epidermis, made up of several layers of keratinocytes (skin cells), constitutes the outer covering of the skin. It is a constantly renewing layer which constitutes the first defense against external aggressions: we speak of a skin barrier. The dermis, for its part, is a vascularized tissue which gives strength and elasticity to the skin via collagen and elastin fibers, produced by cells called fibroblasts.
In the case of severe burns, the loss of the skin barrier leads to loss of fluid and heat as well as a greater risk of infection.
The traditional treatment of deep burns consists of covering them with healthy skin taken from another part of the body: this is autograft. This intervention does not pose any particular technical difficulty, however, in the case of very extensive burns on the body, the problem comes from the fact that there is not enough healthy skin to remove to cover all of the burned areas. .
Making skin in the laboratory
Researchers therefore turned to tissue engineering to make skin tissue in the laboratory. The classic tissue engineering technique is based on the in vitro growth of cells associated with a scaffold (biocompatible porous material). To put it simply, healthy cells are taken from the patient and then cultured and multiplied in order to obtain a sufficient number for seeding on the scaffold. Finally, the seeded cells are allowed to mature until biological tissue is formed .
This technique may, however, present limitations because the spatial distribution of the seeded cells remains difficult to control, particularly when several cell types are used in the same structure.
In response, for several years, bioprinting has emerged as a new tissue engineering technique making it possible to produce biological tissues in a more precise manner (therefore more functional tissues), reproducible and automated.
3D bioprinting
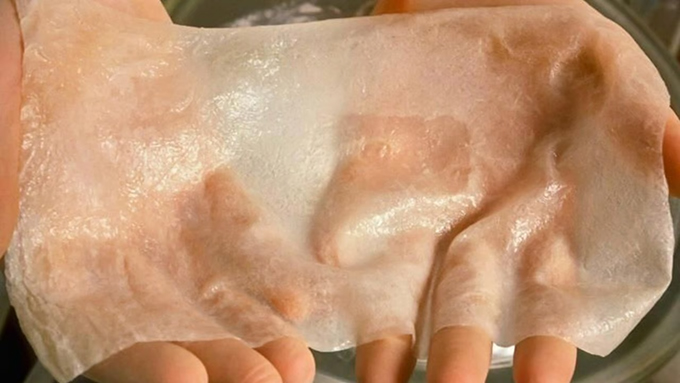
Indeed, thanks to 3D bioprinting, researchers have been able to create three-dimensional skin structures by filling, layer by layer, with a biological ink containing human skin cells (keratinocytes and fibroblasts) suspended in a gel. .
In reality, 3D bioprinting differs little from 3D printing or additive manufacturing used in the industrial sector, for example. Its uniqueness comes from the fact that bioprinters apply layers of biomaterials (bio-ink), which can contain living cells, to create complex structures such as skin tissue.
In the case of severe burns, the objective is to use cells from the patient in order to avoid any potential graft rejection.
The bio-ink consists of two distinct parts: a matrix and the cells of interest taken from the patient. The matrix must allow cells to live, develop and organize themselves. It is generally composed of biocompatible hydrogels such as alginate (polymer from brown algae), gelatin and fibrin (proteins) or even collagen (protein which promotes cell adhesion). The cells of interest, fibroblasts and keratinocytes, are isolated from a biopsy of healthy tissue from the patient.
Once the bio-ink has been formulated, manufacturing skin by 3D bioprinting requires different stages, namely computer-aided design (CAD) of the architecture of the tissue to be printed and bioprinting itself. During the conceptualization stage, CAD, it is necessary to define the spatial organization of all the constituents of the tissues (taking inspiration from the organization of the tissue observed by imaging for example) and the printing parameters of the bio-inks (height of biomaterial layers, printing speed, etc.).
Next comes the automated printing stage of the skin by the printer, which differs depending on the technology used. There are three main technologies: laser printing, microextrusion technology and inkjet technology, each with advantages and disadvantages.
The inkjet technique is strongly inspired by 2D printing on paper. The principle is based on the ejection of microdroplets of bio-ink using a thermal or piezoelectric process. In the first case, a thermal pulse causes the formation of a pocket of steam which causes the ejection of ink droplets by pressure. In the second process, a voltage applied to a piezoelectric crystal causes a mechanical deformation which will compress the ink reservoir and allow the ejection of droplets.
The microextrusion technique uses two print heads (microsyringes), one depositing layers of a hydrogel and the other cells, alternately. These constituents are pushed mechanically through the syringes like gouache coming out of its tube.
Finally, laser printing is the most recent. This time, the ink is spread on a glass slide. A laser strikes it and emits pulses (of the order of a nanosecond) which, absorbed by the ink, allow microdroplets to be detached. This technology is very precise because it allows the placement of the drop to be controlled at the cell level. In addition, it offers the best viability for cells (approximately 95%).
Towards use in hospitals?
Following printing, the printed fabric undergoes a maturation phase where the fabric evolves on its own in a culture medium. This phase allows cells to self-organize until specific biological functions emerge with a view to transplantation. In fact, the maturation stage aims to transform passive living tissue into active living tissue.
This stage of maturation is regulated by the status of innovative therapy medicinal product which is binding.
Finally, once the skin has been obtained, it remains to be grafted onto the patient… This dream is not very far away. Indeed, the company Poietis, a French specialist in 3D laser bioprinting, installed the first 3D bioprinting platform at the end of 2021 for the manufacture of implantable biological tissues at the Assistance Publique – Hôpitaux de Marseille. The first clinical trials are underway.
Author Bio: Coralie Thieulin is a Professor and Researcher in Physics at ECE, doctor in biophysics at ECE Paris
